Probiotics are live beneficial bacteria, which are present in certain supplements and foods. Prebiotics are a kind of fiber present naturally in certain foods such as fruits, vegetables, and legumes. They form food for the probiotics and gut microflora.
Both probiotics and prebiotics are quite talked about topics these days. Though both of them sound similar, they have different roles to play in the maintenance of your health. This article provides information regarding the two.
What is human microbiota?
A large number of fungi, viruses, bacteria, and other types of single-celled organisms reside on your body. All of these consists of the human microbiota. The microbiome refers to all the genes present in the cells of these microbes. According to estimates, every person harbors about 10 trillion to 100 trillion microbial cells that have a symbiotic relationship with the host. As long as your body is healthy, this relationship benefits both the host and the microbes.
The largest number of microbes lives in your gut and this is known as the gut flora (or gut microflora, gut microbiota). Apart from the gut, microbes also reside in your genitals and on your skin and are known as skin flora. The microbiota plays a vital role in immunity and nutrition and may have an effect on your behavior and brain function.
Probiotics
According to the World Health Organization (WHO) probiotics are “live microorganisms which when administered in adequate amounts confer a health benefit on the host.” Probiotics are generally bacteria; however, certain forms of yeasts may also act as probiotics. As the majority of probiotics are bacteria, they are also referred to as ‘friendly bacteria.’
You can obtain probiotics from fermented foods and supplements. Some of the probiotic foods are kefir, yogurt, kimchi, tempeh, and sauerkraut.

A wide variety of probiotic bacteria provide health benefits. The common groups are Bifidobacterium and Lactobacillus. Each group contains many different species of bacteria and many strains are present in each species.
Certain supplements-referred to as multi-probiotics or broad-spectrum probiotics-contain many different species of probiotic bacteria in one product. Interestingly, different probiotic bacteria address different types of health conditions. Hence, it is important to choose the right types or type of probiotic.
How do they work?
As already mentioned, your gut contains a complex variety of microorganisms that is referred to as the gut microbiota. According to estimates, about 1000 different kinds of microorganisms are present in your gut. These include bacteria, viruses, and yeasts; though the vast majority of these are the bacteria. While some of these microorganisms may be harmful to your health, most of them are highly beneficial and even essential to maintain the health of your body.
The majority of the gut microbiota is present in your large intestine or colon. It performs many functions, which are important and essential for your health. Your gut microbiota is very sensitive to what you eat and according to studies, the unbalanced gut microbiota may lead to numerous diseases. Some of these diseases are obesity, metabolic syndrome, type 2 diabetes, colorectal cancer, depression, Alzheimer’s disease, and heart disease.
Benefits and Side Effects of Probiotics
Probiotics work by helping correct the balance of the gut flora and ensuring that these microorganisms perform optimally. Probiotics also help regulate inflammation and protect the skin against pathogens. Skin probiotics play a significant role in improving skin health. Probiotics can help in maintaining your health by:
- Reducing the total number of harmful or bad bacteria in the gut that may cause inflammation or infections.
- Stabilizing the barrier of your digestive tract against harmful bacteria or by making substances that stop their growth.
- Restoring the balance of good vs bad bacteria in the body; thereby, ensuring that your body function optimally.
- Replacing the lost good bacteria of the body; for instance, after taking a course of antibiotics, as antibiotics destroy all the bacteria in the gut (both good and bad). If you do not replace the good bacteria, then there will be an imbalance of good versus bad bacteria in your gut, which may lead to opportunistic gastrointestinal infections.
- They improve skin conditions like atopic eczema, healing of scars and burns, atopic dermatitis, skin’s overall immunity, and its rejuvenating capability. Evidence shows that bacterial cell wall fragments, dead bacteria, and metabolites can prompt specific immune responses in the skin. They also improve skin barrier functions.
What can upset the balance of microflora in the body?
Dysbiosis is the interruption of the balance of the microflora in your body. Dysbiosis of the gastrointestinal tract may occur due to the following reasons:
- An increased intake of sugar, food additives, or protein
- An increased intake of a diet high in highly-processed foods and low in dietary fiber
- Accidental consumption of chemicals such as the remains of a pesticide on unwashed fruits
- Taking medicines such as antibiotics that may affect the gut flora
- Drinking alcoholic beverages daily (two or more)
- Having poor oral hygiene that disrupts the balance of bacteria in your oral cavity (mouth)
- Having high levels of anxiety or stress chronically, which may weaken the immune system and lead to inflammation
- Having unprotected sex that may expose you to disease-causing bacteria

Dysbiosis may also occur on the skin. It can occur due to getting exposed to bad bacteria or when one type of bacteria overgrows on the skin. For instance, there may be an overgrowth of Staphylococcus aureus leading to a staph infection. Similarly, Gardnerella vaginalis bacteria may outgrow healthy vaginal bacteria and cause symptoms of vaginal itching, discharge, and burning.
Signs that you need probiotics
The following are the signs that indicate that you need probiotics:
Gastrointestinal and digestive problems
Stomach disturbances such as gas, constipation, bloating, heartburn, and diarrhea can all indicate that you have an imbalance of your gut flora. A gut that has a balanced flora has less difficulty in processing and digesting food and removing waste.
Increased cravings of sugar
As already mentioned eating a diet rich in added sugars and processed foods can reduce the number of good or friendly bacteria in the gut. This bacterial imbalance can result in increased cravings for sugar that may damage your gastrointestinal tract further. A diet that is rich in refined sugars, especially high-fructose corn syrup may increase inflammation that may lead to numerous diseases including cancers.

Constant fatigue or sleep disturbances
An imbalance of gut flora may result in sleep disturbances including poor sleep or insomnia, and; hence lead to constant and chronic fatigue. Your gut produces the major amount of serotonin required by your body (serotonin is a hormone, which affects sleep and mood). Hence, damage to the gut may negatively affect your sleep. Sleep disturbances are associated with a risk of developing fibromyalgia.
Unintentional changes in weight
Losing or gaining weight without any dietary changes or making changes in your exercise routine may indicate that you have an imbalance of gut flora. The later may impair the ability of your body to absorb essential nutrients, store fat, and regulate levels of blood sugar. Loss of weight may occur due to SIBO (small intestinal bacterial overgrowth), whereas gain in weight may occur due to an urge to eat more (as a result of reduced absorption of nutrients) or insulin resistance.
Skin irritation
Certain skin conditions such as eczema may occur as a result of an imbalance of gut flora. The resulting inflammation in your gut that occurs due to food allergies or eating a poor diet may lead to increased leakage of some proteins from the gut into your body. This can irritate your skin and result in skin conditions including eczema. You may also develop skin conditions such as rashes, hives, and other allergic reactions of the skin.
Candida (yeast) overgrowth
A certain amount of yeast is present in the body of every person without causing any harm. However, due to imbalanced gut flora, the yeast may start overgrowing in your body. Yeast overgrowth can happen at various places in your body. When it occurs in the throat, it may produce symptoms of a sore or itchy throat. Yeast overgrowth on the tongue is a potential cause of bad breath, while in the ears it can produce severe itching and pus in the ear canals. Yeast overgrowth in the genital areas may cause recurrent yeast infections in both males and females. In the folds between your fingers, arms, and back of the knees it may cause eczema-like symptoms. If you get recurrent yeast infections that are not relieved by taking medicines, then you may try taking probiotics. You should also reduce your sugar intake as yeast feeds on sugar or glucose to sustain its growth.
Anxiety and depression
An imbalance of gut flora may lead to symptoms of anxiety, depression, and difficulty staying focused. Your brain and gut are closely connected. Taking probiotics may help in relieving your anxiety and depression and stabilizing mood swings.
Weak immune system
Another sign that indicates that you need probiotics is a weakened immune system. It may manifest as recurrent bouts of cold, flu and other respiratory infections.
Food intolerances
Food intolerance occurs due to difficulty in digesting certain food-items. It is different from a food allergy that occurs due to a reaction of the immune system to some foods. It is believed that food intolerance may occur due to the poor quality of gut flora. This may result in difficulty in digesting and assimilating the trigger food-items and produce unpleasant symptoms including gas, bloating, nausea, abdominal pain, and diarrhea. Some evidence suggests that there is a relationship between food allergies and gut health.

What are the different types of probiotics?
The probiotics that people most commonly ingest are strains belonging to two major species. These two species are also the ones on which most research about probiotics is done.
Bifidobacterium
This bacterial species is commonly utilized in probiotic supplements and foods. It is present in dairy products and also in large amounts in the GI tract of both formula-fed and breastfed infants. They may help by:
- Supporting your immune system
- Limiting the growth of bad or disease-causing bacteria in your intestine
- Helping in the breakdown of lactose into those nutrients that your body may use
The following are the different strains of Bifidobacterium:
B. bifidum
This probiotic strain is the main bacterial strain present in healthy colons, but its level decreases with increasing age. It is also present at low levels in the gut of infants who have allergies. It helps in modulating your immune system and supporting healthy levels of gut flora in people taking antibiotics.
B. longum
This probiotic strain is among the most dominant species of Bifidobacterium that is present in your gut and probiotic products. It helps in reducing inflammation in people suffering from ulcerative colitis. There are two subspecies of this probiotic:
- Bifidobacterium longum subspecies longum (B. longum)
- Bifidobacterium longum subspecies infantis (B. infantis)
B. infantis
This probiotic strain is most commonly present in the gut of infants, but is seldom present in the gut of older adults. According to research, B. infantis may be beneficial in relieving symptoms of IBS and reducing inflammation in people suffering from ulcerative colitis. Another important function of this probiotic strain is that it can metabolize HMOs (human milk oligosaccharides). HMOs are long-chain carbohydrates that are uniquely present in breast milk in high amounts. B. infantis is the only Bifidobacterium strain that can metabolize HMOs.
HMOs have an important role to play in a growing infant due to their prebiotic properties, i.e. they stimulate and support the growth of B. infantis in the gut of the infant. The later is important to establish a healthy gut flora in a breastfed infant.
B. infantis also help in protecting against necrotizing enterocolitis- a serious and life-threatening disease that affects the intestines of premature babies. This probiotic strain is commonly present in probiotic supplements, used in the production of fermented foods (such as cheese, sauerkraut, and yogurt), and added to infant formulas.
Lactobacillus
This is one of the most common probiotic bacteria. It may be present in yogurt and other types of fermented foods. These bacterial species produce lactase, an enzyme that helps in the breakdown of milk sugar or lactose. They also make lactic acid that helps in controlling the growth of disease-causing bacteria. It also forms fuel for your muscles and increases the absorption of minerals by your body. Lactobacillus is naturally present in your mouth, vagina, and small intestines. Each strain of Lactobacillus performs a specific and different functions in your body. The following are the different strains of Lactobacillus:
L. acidophilus
It is a probiotic strain that is highly resistant to breakdown by digestive enzymes. It is generally present in your vagina and small intestines. It plays a role in the digestion of lactose and other polysaccharides, prevents the growth of disease-causing bacteria, and reduces the concentration of cancer-causing enzymes in your intestines. L. acidophilus may be present in fermented soy products such as miso and yogurt.
L. bulgaricus
It is a probiotic strain that is closely related to L. acidophilus. It is used in the production of cheese and yogurt. L. bulgaricus is present in your gastrointestinal tract or gut and helps in keeping it healthy.
L. rhamnosus
It is a probiotic strain that has gut-protective functions. L. rhamnosus GG (LGG) is among the most widely used probiotic strain. It has many well-documented clinical benefits such as treating and preventing gut infections and diarrhea caused by pathogens such as rotavirus, Escherichia coli, Candida species, and Clostridium difficile. This is due to its exceptional ability to stick to surfaces of the gastrointestinal epithelial cells.
L. reuteri
This probiotic strain is usually present in the intestines and mouth. It may prove to be beneficial in relieving symptoms of acute onset infectious diarrhea. This is a type of diarrhea that occurs suddenly as a result of gut infection and lasts for a few days; for instance; food poisoning. Another probiotic that may help in relieving acute diarrhea is LGG. Between LGG and L. reuteri, the former is more effective in reducing both the severity and duration of acute diarrhea.
L. casei
This probiotic strain also has immunomodulatory and gut-protective effects. It acts against the H. pylori bacteria that may infect the stomach and cause gastritis and stomach ulcers. L. casei also helps in protecting and regulating immunity of the intestinal mucosa. By its action, it reduces the entry of mucosal pathogens into your bloodstream.
L. plantarum
This probiotic strain supports the health of your GI tract by preventing alterations in the population of gut flora. It helps in preventing the entry of pathogens into your bloodstream from the gut by ensuring that your intestinal barrier function is intact. It also inhibits the action of Clostridium difficile (C. difficile), a bacterium that may cause a range of problems ranging from diarrhea to colitis. The elderly and people who take antibiotics for long duration are at an increased risk of getting C. difficile infection. People who suffer from irritable bowel syndrome also take L. plantarum to promote healthy levels of gut flora.
Saccharomyces boulardii
This is a kind of non-pathogenic probiotic yeast. It can improve the functioning of your GI lining. Hence, it helps in protecting against and treating various types of diarrhea such as traveler’s diarrhea and antibiotic-associated diarrhea and other issues of the digestive tract such as C. difficile infection, H. pylori infection, parasitic infections, and IBS.
Prebiotics
Prebiotics are a kind of nutrients, which your body can’t digest. They form as food for probiotic microorganisms or the good bacteria in your gut. They are equally important for your body as probiotics. They play a vital role in the absorption of nutrients and the maintenance of digestive health. They are also referred to as superfoods or fertilizers as they are the nutrient or food source for the gut flora (good bacteria). Foods that are rich in fiber such as vegetables, whole grains, and fruits contain prebiotics.
There are different types of prebiotics, most of them being a subset of carbohydrate groups, which are mainly oligosaccharide carbohydrates (OSCs). The following are the different types of prebiotics:

Fructans
Under this category comes the prebiotics fructo-oligosaccharide (oligofructose) and inulin.
Galacto-oligosaccharides (GOS)
They can stimulate Lactobacilli and Bifidobacteria greatly.
Glucose and starch-derived oligosaccharides
There is a type of starch, which is resistant to digestion by the upper gut and is referred to as resistant starch (RS). It may promote health and is a type of prebiotic. An example of an oligosaccharide derived from glucose is polydextrose.
Other oligosaccharides
Some of the oligosaccharides originate from a polysaccharide referred to as pectin and are known as pectic oligosaccharide (POS).
Non-carbohydrate oligosaccharides
There are certain compounds, which are not carbohydrates but are classified as prebiotics; for instance; cocoa-derived flavanols.
Benefits and Side Effects of Prebiotics
The beneficial effects of probiotics are linked to the beneficial effects of prebiotics. Taking prebiotics may promote a healthy GI tract; thereby, offering better digestion, fewer health problems related to antibiotics, and many other benefits. According to research prebiotics may provide the following health benefits:
- Improve absorption of calcium; thereby, increasing bone density.
- Support the growth of gut flora; hence, promoting digestion and overall metabolism.
- Change the speed at which the body may process carbohydrates. When your body is not able to metabolize sugars properly, it may lead to inflammation, which is one of the common causes of ischemic heart disease.
- Reduce insulin resistance.
- Maintain the levels of minerals and electrolytes (such as sodium and potassium) in your body. This helps in controlling the blood pressure.
- Promote better hormonal balance that results in less stress.
Comparison between prebiotics vs probiotics.
| PREBIOTICS | PROBIOTICS |
|---|---|
| Prebiotics are a special type of plant fiber that promote the healthy microorganisms or probiotics that are already present in the digestive system. | Probiotics are live microorganisms – bacteria or yeast – that are found in certain fermented foods, supplements and skin care products |
| Prebiotics support smooth and healthy digestion and prevent constipation. They also support prebiotics in performing their functions. | Probiotics support the health of the gastrointestinal tract, skin health and boost the body’s immune system |
| Prebiotics are not active living organisms and are therefore unaffected factors such as stomach acid content and heat. They can stay for longer periods in the body | Probiotics are sensitive to the amount of stomach acid and heat. These factors can kill the active healthy bacteria |
| Good natural sources of prebiotics include garlics, onions, fruits, vegetables, legumes and leeks. | Good natural sources of probiotics are yoghurt, kimchi, buttermilk, kimchi, sourdough bread, sauerkraut, tempeh and kombucha |
| Key prebiotics are insoluble plant fibers – complex carbohydrates like glucose and starch derived oligosacharides. | Key probiotics include several strands of the Lactobacillus bacteria which includes L. acidophilus, L. bulgaricus, L. rhamnosus, L. plantarum, etc. |
How prebiotics and probiotics work?
The use of probiotics and prebiotics together is referred to as microbiome therapy. It is not necessary to take probiotics with prebiotics for the former to work. But, taking them together may increase the effectiveness of your probiotics. Prebiotics or the promoters of good bacteria and probiotic microorganisms work synergistically. As prebiotics travel down the gut, they encourage the growth and survival of probiotics. This helps in restoring and improving the health of your gut and other internal organs of the body. Products, which combine these two, are known as synbiotics.
What are the general benefits of taking probiotics?
Probiotics promote the health of your gut flora and provide multiple health benefits. Some of the general benefits of taking probiotics are:
They help in balancing the good bacteria in your GI tract
One of the main health benefits of taking probiotics is that they help in restoring the balance of gut flora. An imbalance of gut flora indicates that there is an excess of bad or harmful bacteria and less amount of good bacteria present in the gut. Due to this, you may suffer from digestive issues, obesity, mental health issues, allergies, and more.

They help in preventing and treating diarrhea
Diarrhea can occur due to a wide variety of causes such as antibiotic use, infections, and traveler’s diarrhea. Probiotic use may help in not only preventing diarrhea but also reducing its severity.
They help in improving certain mental health issues
According to research, taking probiotics can help in improving symptoms of certain mental health problems such as anxiety, stress, depression, and memory.
Certain strains of probiotics may help in maintaining the health of your heart
Taking probiotics can help in protecting your heart by decreasing the levels of LDL (bad) cholesterol and reducing blood pressure modestly.
They may help in reducing the severity of eczema and allergies
Certain strains of probiotics may help in reducing the severity of some allergies like eczema in infants and children.
They may help in reducing the symptoms and signs of certain disorders of the GI tract
Taking probiotics can help in reducing the symptoms and signs of GI disorders such as irritable bowel syndrome, necrotizing colitis, and inflammatory bowel disease (ulcerative colitis).
They may help in boosting the immune system
Taking probiotics can provide a boost to your immunity and prevent against infections such as respiratory infections and urinary tract infections.

They may help you in losing belly fat and weight
Certain strains of probiotics can help in losing weight through many different mechanisms. For instance, some probiotic strains work by preventing the absorption of fat in the intestines. This fat then gets excreted by way of feces instead of getting stored in your body. Probiotics can also help you lose weight by making you feel full for a longer time, storing less fat, and burning more calories.
What are the benefits of taking probiotics for skin?
For your skin, probiotic microorganisms work in a very similar manner as they work for your digestive system. They help in keeping your skin in a balanced condition. At a superficial level this is expressed as skin, which is neither too oily nor too dry, and skin which can repel the inflammation-causing environmental conditions effectively.
The gut-brain-skin-axis theory is quite old and it believes that your emotional state including stress, depression or anxiety may alter the functioning of the gut and cause a buildup of unhealthy or bad bacteria. This causes inflammation leading to flare-ups and breakouts in people with skin problems including acne, eczema or Rosacea.
Probiotics help to create a healthy GI tract so that less amount of toxins gets absorbed in your bloodstream. Toxins prevent the absorption of essential nutrients, minerals, and vitamins; thereby, interfering with the ability of your body to remove waste products, causing inflammation.
When you apply them topically, probiotics can provide many benefits to your skin. They provide a protective barrier to your skin and prevent harmful microorganisms from triggering an immune reaction. This helps in combating inflammation and creating a calmer environment for your skin. Probiotics also produce antimicrobial peptides-the natural antibodies-that help in combating harmful bacteria. Furthermore, they also help in enhancing the functionality of the skin to deal with external environmental factors that may damage it including sun, pollution, and free radicals. All these benefits help in reducing inflammation and flare-ups of skin conditions, and preventing the signs of premature aging.

Premature aging
Gut flora helps in eliminating toxins from the body; thereby, preventing inflammation and appearance of signs of premature aging on your skin. Taking probiotics helps in not only flushing out bodily toxins but also repairing the damage due to free radicals. Topical application of probiotics enhances better absorption of moisture and delays premature signs of aging such as fine lines and wrinkles. Lactic acid bacteria help in reducing the appearance of fine lines and wrinkles and tightening pores. They also possess exfoliating properties to improve dull and dry skin and nourishing properties to soothe damage due to sun exposure. Furthermore, it was found that skin creams containing Streptococcus thermophiles increased moisture content in the skin of aging women. This implies that probiotics help your skin to retain moisture. A skin that is well-hydrated has less visible wrinkles.
Topical probiotics also help to strengthen the barrier function of the skin. Your skin is a physical barrier that safeguards your internal organs by keeping out disease-causing pathogens and other toxins. The skin microflora protects against damage from harmful bacteria, free radicals, and pollution all of which can accelerate the process of aging. It also helps to limit your exposure to UV rays of the sun and allergens. Both of these may cause damage to your skin and result in premature aging.
Some evidence exists to prove that taking probiotics may help in building collagen, which is the major skin protein affecting its tone and texture.
Acne
Small studies show that probiotics that you consume in the form of supplements or food along with standard treatments for acne may raise the rate of clearance of acne lesions. Some of the probiotic strains that are effective against acne in studies include B. bifudum, Lactobacillus, and L. acidophilus. Some more studies have shown that consumption of non-fermented pasteurized dairy is associated with acne, whereas fermented dairy is not. Oral probiotics reduce systemic markers of inflammation and oxidative stress. There is an elevation of these markers in people suffering from acne. Furthermore, oral probiotics also regulate the release of pro-inflammatory cytokines in the skin.
Topical probiotics may also decrease the total number of active acne lesions as seen in preliminary studies. When you apply probiotics to your skin they help acne lesions by acting as a protective barrier and prevent acne-causing bacteria from entering your skin, aggravate your immune system, and trigger inflammation.

Rosacea
This is an inflammatory condition of the skin in which redness occurs on your cheeks, nose, forehead, or chin along with small red pimples or bumps. According to studies, probiotics may help in controlling symptoms and flare-ups of Rosacea when taken orally or applied topically to the affected areas of the skin. Probiotic extracts along with medicine may help in reducing the redness of Rosacea and improving and strengthening the skin barrier; thereby, reducing its burning, dryness, and stinging.
One home remedy that you may try to relieve symptoms of Rosacea is making kefir face masks. Many people claim that applying a kefir face mask to the skin with Rosacea is very soothing and calming. Kefir is a type of fermented milk that is a rich source of probiotics. It contains many beneficial strains of probiotic bacteria and yeasts. Kefir also has the additional benefit of containing lactic acid that has anti-aging properties.
Eczema
Eczema is a skin condition in which your skin becomes red, dry, itchy, and cracked. In a Finnish study, researchers observed pregnant females who consumed probiotic supplements (with Lactobacillus rhamnosus GG) for 2-4 weeks before delivery and post-delivery in case they breast-fed their babies. Researchers also added the probiotic to infant formula and babies took it for a minimum of six months. It was found that probiotics decreased the risk of eczema in infants with a strong positive family history of the condition.
Another recent clinical study shows that in infants who had eczema before they turned one year old, the collection of gut flora was less diverse while they were seven days old in comparison to infants who didn’t have eczema. This suggests that a link exists between the quality of gut flora during early life and the occurrence of eczema. The yeast strain of Saccharomyces boulardii is specifically found to be useful to improve symptoms of eczema.
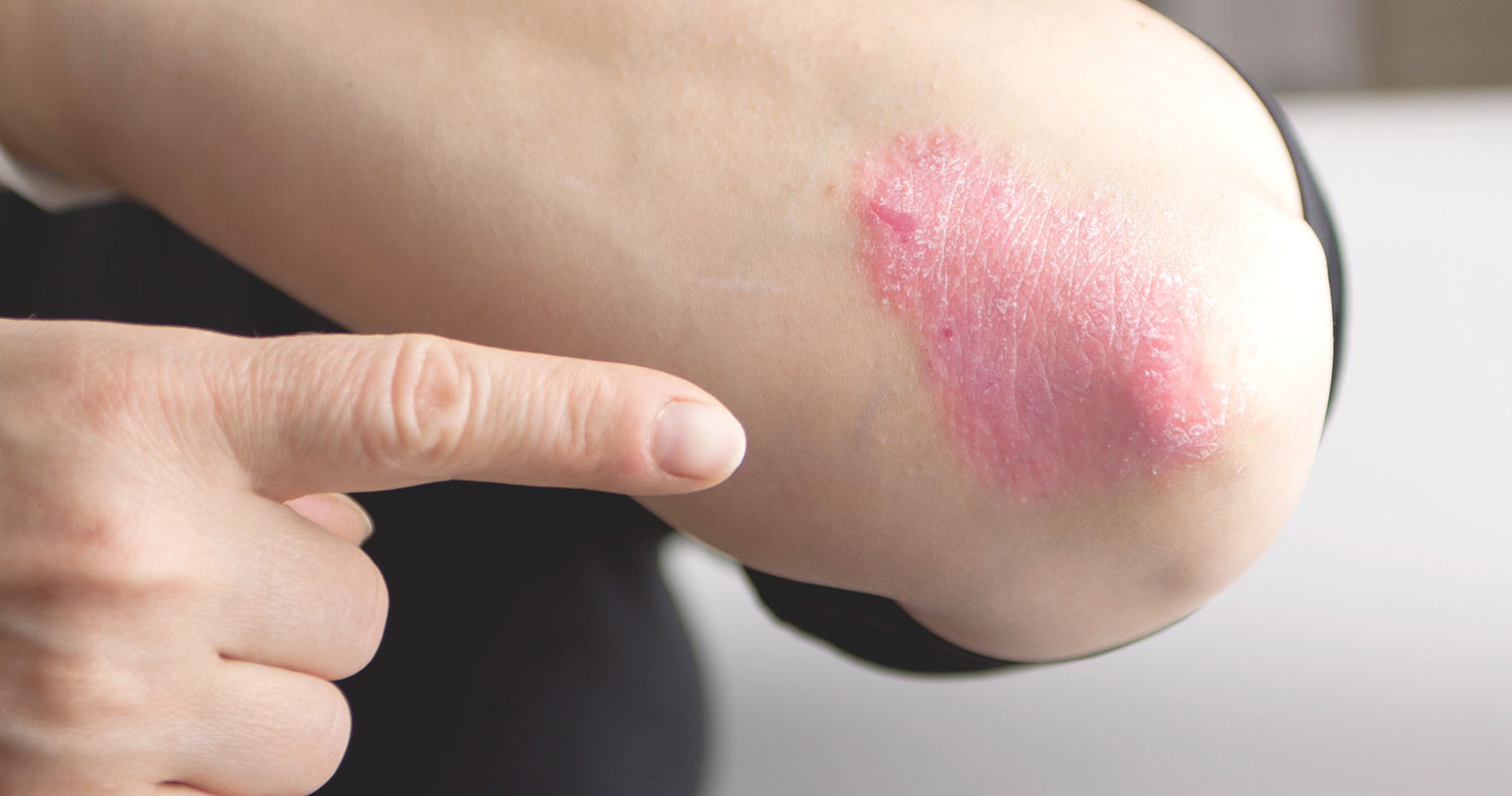
Psoriasis
Psoriasis is another type of skin condition linked to inflammation. Consuming probiotics may prove to be beneficial if you suffer from psoriasis. The strains that are particularly beneficial in relieving symptoms of psoriasis are Lactobacillus acidophilus, L. rhamnous, L. lactis, Bifidobacteria longum, B. bifidum, and Streptococcus thermophilus.
Where can you find probiotics?
You may find probiotics in the following:
Food
Fermented foods including kefir, yogurt, kimchi, miso, sauerkraut, and tempeh.
Probiotic supplements
These are available either in the form of capsules or powders. The exact dose, means of delivery, and the period of viability of probiotics may vary with the strain you are consuming and the condition for which you are taking them.
Skin care products
Topical creams, lotions, cleansers, and moisturizers. Nowadays, you may find probiotics such as lactic acid bacteria in many of the topical skin care products.
Relationship between probiotics, gut microbiome and, skin flora
Your gut microbiome is a huge collection of various types of bacteria, fungi, protozoa, and viruses that colonize your GI tract. The gut microflora provides vital immune and metabolic benefits to the host. It helps in the breakdown of complex polysaccharides and plays an important role in the production of some nutrients such as vitamin K. It protects against environmental pathogens both directly and indirectly (directly by attaching to the epithelial cells thus providing competition, and indirectly by triggering immune responses).
When your skin is in a state of perfect balance or homeostasis, it performs its various functions such as protection, water retention, temperature regulation, etc. effectively. Your gut microflora has an effect on maintaining the state of homeostasis of the skin. Furthermore, the gut microflora also influences the skin microbiome or skin flora. It has been documented in various human and rodent studies that gut bacteria have a beneficial effect on your skin health.

The gut microflora can contribute to skin allostasis, which is the restoration of the state of homeostasis of the skin after a stressor or disturbance. It has also been found that the gut microflora can restore homeostasis of the skin after exposure to ultraviolet rays.
Intestinal dysbiosis, a condition in which there is a microbial imbalance in the gut can negatively affect skin function. This can contribute to the occurrence of three common disorders of the skin: atopic dermatitis (eczema), psoriasis, and acne.
Your diet has a great influence on the gut microflora and in turn on the skin flora. Taking probiotic supplements may help in the management and prevention of various skin disorders including psoriasis, atopic dermatitis, and acne vulgaris. Prebiotics and synbiotics-a combination of probiotics and prebiotics- provide similar health benefits.
References
https://www.healthline.com/nutrition/probiotics-101
https://my.clevelandclinic.org/health/drugs/14598-probiotics
https://www.ncbi.nlm.nih.gov/pubmed/12583961
https://www.ncbi.nlm.nih.gov/pubmed/24365095
https://www.ncbi.nlm.nih.gov/pubmed/20664075
https://www.healthline.com/health/digestive-health/dysbiosis#causes-and-risk-factors
https://www.healthline.com/health/gut-health#signs-and-symptoms
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6463098/
https://www.medicalnewstoday.com/articles/323490.php
https://www.healthline.com/health/prebiotics-vs-probiotics
https://www.eatright.org/food/vitamins-and-supplements/nutrient-rich-foods/prebiotics-and-probiotics-creating-a-healthier-you
https://www.healthline.com/nutrition/8-health-benefits-of-probiotics#section2
https://www.dermstore.com/blog/top_ten/benefits-of-probiotics-for-skin/
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3038963/
https://www.vogue.com/article/probiotic-prebiotic-skin-care-guide-dermatologist-expert-tips
https://www.livescience.com/46502-probiotics-hold-promise-skin-conditions.html
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6048199/
https://www.medicalnewstoday.com/articles/307998.php







