Have you looked at your friend’s glowing complexion and wonder what’s the secret to that glow? Is it a product which she is using and you are not? Well, there are many reasons for this. It could be your friend is blessed with good genes or is conscientious in her skincare regime. But what is not known to many is that the key to healthy skin is a healthy gut.
Hence instead of saying “you are what you eat”, we should be saying “you are what you absorb”. This is because our gut and brain share a close connection, a concept known as the gut-brain connection.

Gut-brain connection
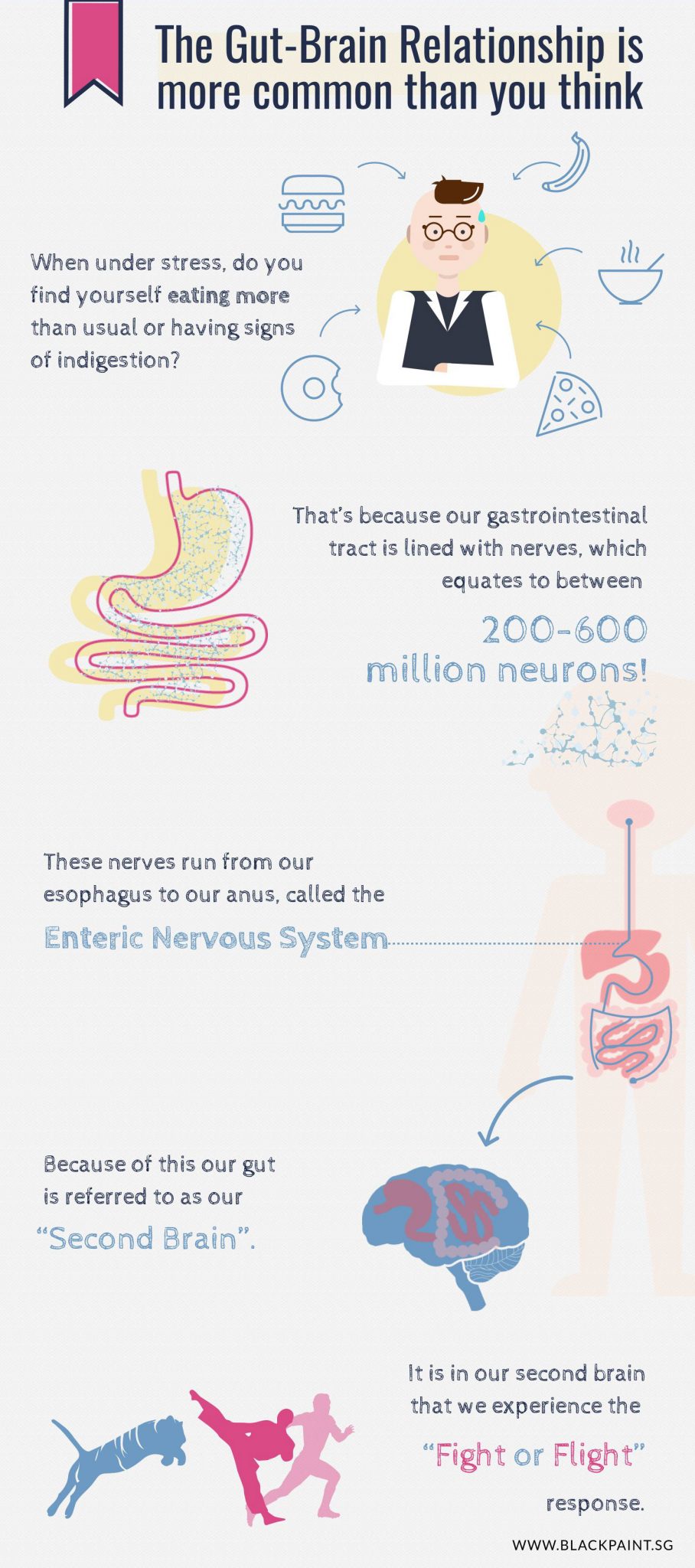
“Gut-brain connection”, also know as “Gut-brain relationship”, may sound like an alien word, but it is not. In fact, most of us refer to this (concept) without knowing it. For example, do you find yourself having the runs when you are tense or nervous? Or when under stress, do you find yourself eating more than usual or having signs of indigestion?
I know when I get stressed, I will experience gastric as well as severe IBS cramps. This is because our gastrointestinal tract is innervated with lots of nerves (specifically 200-600 million neurons!), and they run from the oesophagus all the way to the anus. This nervous system is called the enteric nervous system and is the reason why our gut is often termed as the second brain.
This second brain is sensitive to life-threatening emotions – i.e. the fight-or-flight response and signals that they pick up will be sent to the other nervous network in our gut – the central nervous system – and execute a response, such as activating the defecation centres (meaning more trips to the loo) or altering gastric juice production via signals sent to the stomach.
Besides reacting to our emotions, we need this enteric nervous system as it ensures good blood flow to the gut and proper food digestion.
Gut microbiome and our emotional and mental health
Another lifestyle example to illustrate this gut-brain relationship would be the role of serotonin and how its levels in our body can affect our mood and sleep. Serotonin is a neurotransmitter produced by our brain and gastrointestinal tract, with the latter being the major serotonin producer. About 80-90% of our body’s serotonin is produced in our gastrointestinal tract.
Low levels of serotonin have been found in people with depression, and it is no wonder that serotonin has been called the “feel-good hormone”. Besides, our brain uses serotonin to make melatonin, the important hormone to help you sleep. Hence, how much serotonin your body makes would have a direct impact on the quality and quantity of your sleep.

Not many people know this, but the population of our gut bacteria has an impact on our emotional and mental health, as well as our ability to get the much-needed sleep at night.
A study involving 40 healthy females have found women with a higher percentage of the Prevotella species of bacteria in their stools were more likely to experience negative emotions after they were shown negative images compared to women with the higher percentage of the Bacteroides species of bacteria in their stools.
Likewise, individuals with autism appear to be more susceptible to gastrointestinal problems such as inflammatory bowel disease and leaky gut, and this could be due to altered gut microbiome composition. However, when these group of individuals was given a certain probiotic strain, it resulted in improved gut barrier integrity, as well as a reduction in abnormal autism-related behaviours.
Lastly, there is a close relationship between our gut bacteria and sleep. The bacteria in our gut help in serotonin production (which then goes on to form melatonin), but did you know that our gut microbiome population can be affected by a lack of sleep or poor-quality sleep? That means to say there is a vicious cycle of sleep deprivation/ poor-quality sleep and poor gut health.
The relationship between our gut and skin is not new. This theory was first suggested by dermatologists, John H. Stokes and Donald M. Pillsbury, at least more than 70 years ago. They suggested there could be an overlapping mechanism between depression, anxiety and skin conditions such as acne.
Stokes and Pillsbury speculated that the microflora in our gut is easily influenced by our emotional states – i.e. feelings of stress, worry, anxiety or depression might upset the normal intestinal microflora population, resulting in increased intestinal permeability (think ‘leaky gut’), which then triggers an inflammatory response throughout our body and skin.
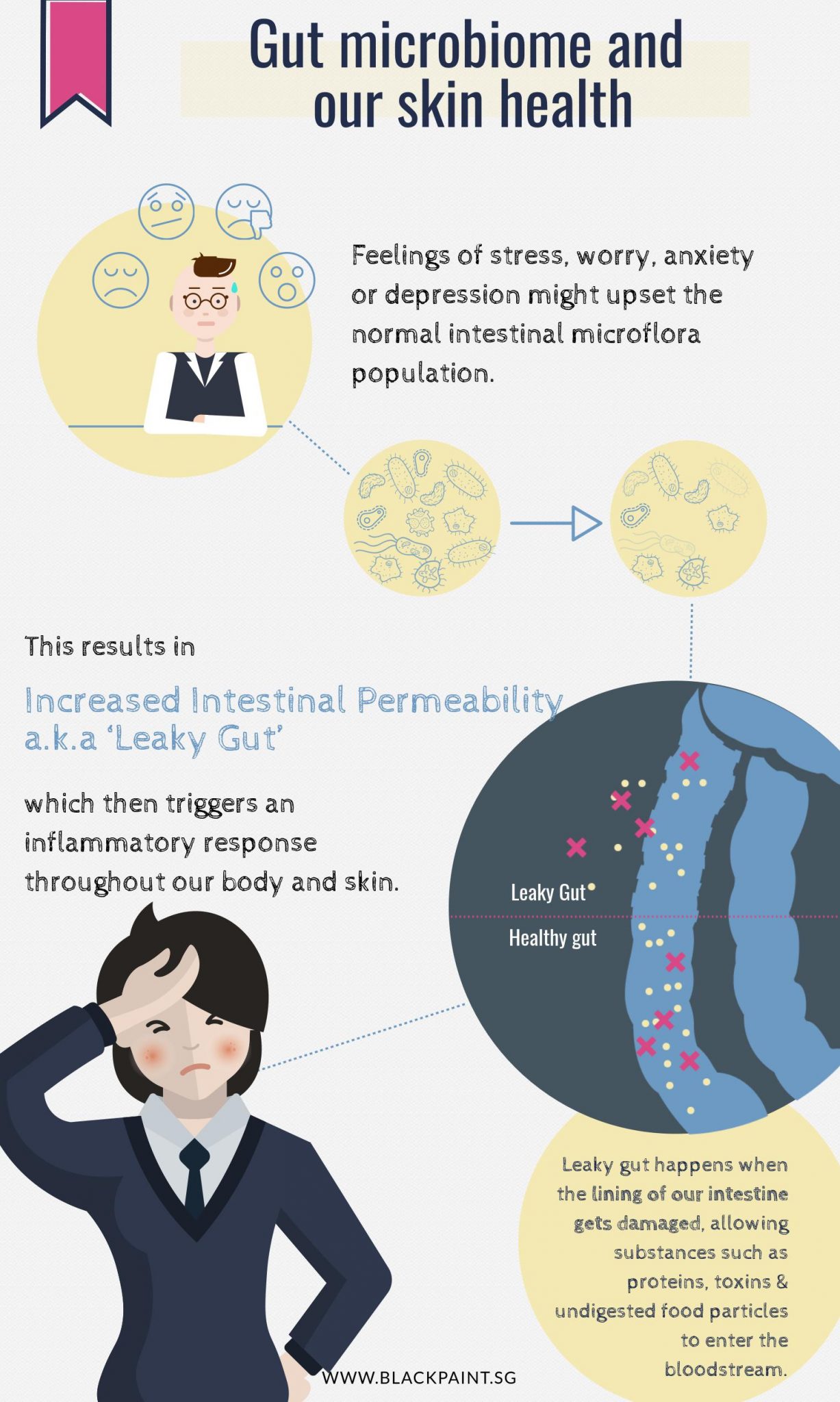
Leaky gut happens when the lining of our intestine gets damaged, allowing substances which it does not normally allow to pass through – such as proteins, toxins, undigested food particles – to enter the bloodstream. Our immune system recognises these substances as foreign, thereby mounting an immune response, which is inflammatory.
What causes leaky gut?
Stress, especially if it is chronic
- Chronic stress is a risk factor for prolonged inflammation.
- Because inflammation is an immune response, hence prolonged immune changes may alter the gut environment, which subsequently affects the gut microbiota population.
Poor quality diet
A diet that is high in processed foods (aka “junk foods”)
Imbalance of gut microbiota (dysbiosis):
The main culprit: prolonged intake of antibiotics
Toxins overload
Mainly due to excessive intake of NSAIDs (e.g. aspirin, ibuprofen), antibiotics
Some symptoms of leaky gut include:
- Skin issues such as acne and rosacea
- Flatulence (bloating)
- Food sensitivities
- Fatigue
- Weight gain

To illustrate the above point, one study involving more than 13,000 adolescents has found gastrointestinal symptoms such as abdominal bloating, constipation and reflux were more common among teens with acne. In addition, it has been recently confirmed that having low stomach acid (medically known as hypochlorhydria) is a huge risk factor for small intestine bacterial overgrowth (SIBO), a condition whereby bacteria from the colon migrate to the small intestine.
Symptoms of SIBO are mild and usually non-specific – abdominal distention, bloating, pain or discomfort, diarrhoea, weakness and fatigue. If left untreated, SIBO can lead to malabsorption and consequently nutrient deficiencies.
Hence it seems clear that a healthy gut is a key to a healthy mind and body. However, it must be kept in mind that these systems do not function in isolation. A healthy gut can help achieve physical and mental health, but a healthy mind is also needed for a healthy gut. As such, there is a complex relationship between our gut, mind and body. Therefore, in order to be in tip-top shape, we need to adopt practices that take care of all these three body systems – brain, gut and overall body.
Here are some lifestyle tips to help you feel and look your best
1. Consume foods rich in probiotics
- These are the live bacteria found in fermented foods such as miso, kimchi, yoghurt.
- Probiotics are often called “good” bacteria as they keep our intestines healthy – i.e. preventing “bad” bacteria from colonising our gut.
- Probiotics can help maintain the integrity of our intestinal lining, thereby preventing against leaky gut.
 2. Eat foods high in omega-3 fatty acids.
2. Eat foods high in omega-3 fatty acids.
- Omega-3 fatty acids are essential fatty acids as our bodies do not make them, meaning they need to be obtained from our diets.
- These fatty acids can help calm the inflammatory process in our body, and help in mood regulation, thereby protecting against mental disorders such as depression, bipolar disease, suicide and self-harm.
- Foods rich in omega-3 fatty acids: oily fish (salmon, cod, sardine), walnuts, flaxseed (also known as linseed), and chia seed.
 3. Eat more bananas, milk, cheese, eggs, fish, sunflower seeds, cereal grains and legumes.
3. Eat more bananas, milk, cheese, eggs, fish, sunflower seeds, cereal grains and legumes.
- These foods are high in vitamin B6, the vitamin important for mental health as it is required for neurotransmitter synthesis.
- Neurotransmitters are chemical messengers responsible for transmitting signals from one neuron (nerve cell) to the next. This is how information is passed throughout our brain and body.
- Our body uses vitamin B6 to make serotonin, the important hormone to help you feel good and sleep well at night.
 4. Eat a diet high in unprocessed, whole foods such as unrefined carbohydrates
4. Eat a diet high in unprocessed, whole foods such as unrefined carbohydrates
- These are wholegrain bread, cereals, brown rice), fruits and vegetables, they are high in dietary fibre, which is important for bowel regularity and timely removal of toxic substances from the body.
- The average recommended dietary intake of fibre is 25-30g a day.
- Fruits and vegetables are also high in vitamins and antioxidants, nutrients needed to fight against free radicals, thereby protecting against collagen breakdown.
 5. Include prebiotics in your diet.
5. Include prebiotics in your diet.
- Good food sources include garlic, onions, unripe bananas, Jerusalem artichokes, wheat bran or any foods containing oligosaccharides such as inulin.
- Prebiotics are indigestible fibre that is needed to support the growth of our gut bacteria.
 6. Keep your emotional health in check.
6. Keep your emotional health in check.
- This means to find healthy ways to deal with your anger or frustration such as talking out with a loved one and engaging in an activity which you enjoy.
- If you find yourself worrying too much, doing up a “to-do” list might be helpful.
 7. Stress management.
7. Stress management.
- Not finding ways to manage stress can have negative consequences such as we find ourselves falling sick more easily, feeling depressed, poor work performance, emotional eating, etc.
- Hence finding ways to deal with that stress can help us stay and perform to our best.
 8. Exercise regularly.
8. Exercise regularly.
- Not only exercise can help in destressing and weight management, but it can also help increase serotonin production in your body.
- Exercise need not always mean hitting the gym; it can be a brisk walk around the neighbourhood or dancing the night away – just make sure it is an activity that gets your body moving and something which you enjoy doing.
 9. Maintain a regular sleep routine.
9. Maintain a regular sleep routine.
- As mentioned earlier, sleep deprivation and/or poor-quality sleep can disrupt the population of bacteria in our gut, which then have a roll-on effect in our overall health.

Here is a recipe for you to try!
Gut-brain friendly five-spice fish with stir-fried vegetables
Ingredients:
- ½ cup brown rice
- ½ cup quinoa
- 1 ½ tablespoon cooking oil (preferably canola or sunflower oil)
- 2 x 180g skinless salmon or tuna fillets, halved to make 4 fillets
- 2 teaspoons Chinese five-spice powder ( 五香粉 )
- 5 button mushrooms or shiitake mushrooms, quartered if small, thinly sliced if large
- 2 garlic cloves, thinly sliced
- 4cm piece size ginger, peeled & grated
- 2 bunches bok choy, quartered
- 1 ½ tablespoons oyster sauce
- 2 teaspoons sesame seeds, to serve

Instructions:
- Mix brown rice and quinoa together and cook according to packet instructions; If cooking on the stove, drain and cover to keep warm and set aside.
- Meanwhile, place a wok (or large non-stick frying pan) over high heat and heat half of the oil. Coat selected fish fillets evenly with Chinese five-spice powder; cook, turning occasionally, for 3–4 minutes, or until fillets are golden brown and starting to flake. Remove cooked fish from the wok, cover to keep warm and set aside.
- Add remaining cooking oil to wok (or pan) with mushrooms, garlic, and ginger, cook, stirring occasionally, for 1–2 minutes, or until mushrooms are soft and the mixture is aromatic.
- Add bok choy and oyster sauce to wok (or pan) with 2 tablespoons water. (The mixture will steam slightly.) Cook vegetables for 2 more minutes, or until greens are bright green and just tender.
- Divide reserved cooked rice among 4 bowls, then top with stir-fried veggies and reserved five-spice salmon; scatter with sesame seeds and serve.
- Enjoy!
(Recipe adapted from Australian Healthy Food Guide magazine, Feb 2015)



 2. Eat foods high in omega-3 fatty acids.
2. Eat foods high in omega-3 fatty acids. 3. Eat more bananas, milk, cheese, eggs, fish, sunflower seeds, cereal grains and legumes.
3. Eat more bananas, milk, cheese, eggs, fish, sunflower seeds, cereal grains and legumes. 4. Eat a diet high in unprocessed, whole foods such as unrefined carbohydrates
4. Eat a diet high in unprocessed, whole foods such as unrefined carbohydrates 5. Include prebiotics in your diet.
5. Include prebiotics in your diet. 6. Keep your emotional health in check.
6. Keep your emotional health in check. 7. Stress management.
7. Stress management. 8. Exercise regularly.
8. Exercise regularly. 9. Maintain a regular sleep routine.
9. Maintain a regular sleep routine.



